Do I Need a Hip Replacement Quiz
Do I Need a Hip Replacement Quiz
If you’re experiencing hip pain and limited mobility, you may wonder if a hip replacement surgery is the right solution. While a hip replacement can be a life-changing procedure that can significantly improve your quality of life, it’s important to know if it’s the right option for you. Taking a quiz to determine if you need a hip replacement is a good starting point to understand if this surgery is necessary.
A hip replacement surgery is a procedure in which a damaged hip joint is replaced with an artificial one. It’s usually recommended for people with severe hip arthritis, hip fractures, or other conditions that cause significant pain and disability. Hip replacements are typically recommended as a last resort when other treatments, such as physical therapy, medication, and lifestyle changes, have been unsuccessful.
A hip replacement quiz can help you evaluate the severity of your hip pain and mobility issues and determine if a hip replacement surgery is necessary. Remembering that a quiz is not a substitute for a proper medical evaluation is important. Only a qualified healthcare professional can make a definitive diagnosis and recommend the most appropriate treatment plan for your specific condition. However, taking a hip replacement quiz can be a helpful first step in understanding your options and determining if a conversation with a medical professional is necessary.
What is a hip prosthesis?
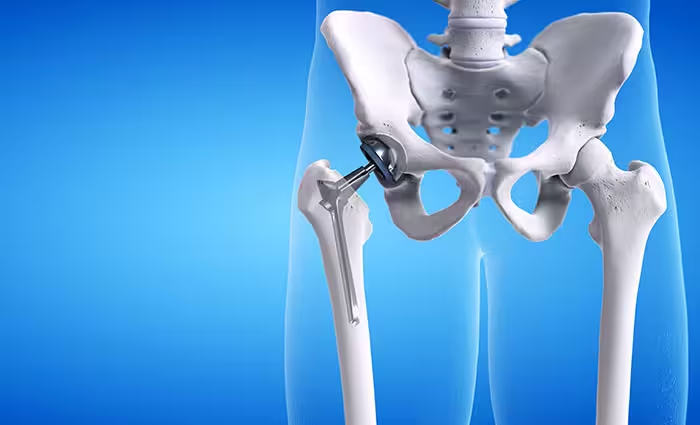
A hip prosthesis or endoprosthesis is an implant that entirely or partially replaces the damaged hip joint. It remains permanently in the body and takes over all functions of the pathologically changed joint. The human hip joint consists of two bony parts, the femoral head, and the acetabulum. The femoral head forms the upper end of the thigh bone and moves in the acetabulum. Between the two parts, the cartilage mass and the synovial fluid ensure very low-friction movement and optimal force distribution to the underlying bone.
When do you need a hip prosthesis?
A hip replacement is used in the following cases, among others:
- In the case of hip osteoarthritis: hip osteoarthritis forms a very common reason for an artificial hip joint. The loss of cartilage causes increasing degeneration of the joint, which ultimately causes limited mobility and severe pain.
- In the case of femoral head necrosis: In this disease, the bone structure in the femoral head loses its vitality due to disturbances in blood circulation. The bone’s death can also affect the joint surface, so an artificial hip joint can provide relief.
- After a fracture of the neck of the femur: An artificial hip joint may also be required due to a fracture of the neck of the femur (e.g., due to a fall).
The hip prosthesis is necessary in case of painful hip arthrosis (coxarthrosis) and displaced femoral neck fractures with impaired blood supply to the femoral head (femoral head necrosis). Hip osteoarthritis is the painful wear of the articular cartilage with bony changes often associated with inflammation of the synovium (synovitis).
Hip osteoarthritis leads to loss of function of the hip joint with noticeable stiffening and significantly impairs the patient’s daily mobility and gait pattern. A hip prosthesis reliably restores this mobility and, to a certain extent, the ability to engage in sports. It also eliminates severe joint pain to a considerable extent.
Although the implantation of an artificial hip joint is nowadays a routine operation, it still requires a great deal of experience on the part of the surgeon due to the individual circumstances of each patient and the variety of available materials, prosthesis types, and fastening techniques.
The goal of prosthetic planning by the orthopedic hip specialist is a durable, well-functioning hip prosthesis that meets the patient’s specific requirements and gives him a ‘natural feeling.’ We are talking about a so-called ‘forgotten hip,’ which provides the patient with a natural feeling that he does not feel any difference in everyday life compared to the non-operated, healthy hip and already forgets about the operation.
Nowadays, a prosthesis should last at least 20-25 years before loosening or wear necessitates a surgical prosthesis change (revision of the hip prosthesis).
The hip specialists at the Joint Clinic optimally adapt the treatment alternatives from prosthesis models, surgical methods, and fastening techniques to the respective patient. When planning and performing hip replacement surgery, they consider specific factors such as age, activity, bone quality, and individual anatomy.
How long does a hip prosthesis last?
Studies on whether sporting activity shortens the service life of a hip prosthesis are still inadequate. It has been proven that trained, strong muscles and regular exercise positively influence general health and can be continued even after the implantation of a prosthesis. Patients should be encouraged to participate in sports with a harmonious, regular sequence of movements, such as cycling or cross-trainer use.
Like other types of prostheses, a hip prosthesis has limited durability. With proper surgery, the lifespan of hip TEP is 20 to 25 years, and in some cases, even longer. Patients older than 65 have a very good chance of not going through a prosthetic replacement in their lifetime.
What helps the lifespan of a hip prosthesis?
- Abstaining from sports that put a strain on the joints, such as skiing or tennis,
- low-impact sports activities such as swimming, cycling, or hiking,
- intensive rehabilitation and extensive muscle building following hip surgery,
- careful planning of individual biomechanics by an experienced surgeon.
What are the risks of hip surgery?
Hip surgery has the same surgical and anesthetic risks as any surgical procedure. Possible complications include, for example, wound healing problems, post-operative bleeding, or bruising. In addition, there is a risk of venous thrombosis during major orthopedic surgery, which is why thrombosis prophylaxis is administered. The latter continues for several weeks after the operation. After the insertion of the artificial hip, infections, calcifications, and adhesions can occur in rare cases. Very rarely, dislocation of the artificial joint, a so-called hip luxation, can occur. In the worst case, a new operation may be necessary.
General surgical risks:
- Infections
- Wound healing disorders
- Postoperative bleeding
- Bruises / hematomas
- Injury to nerves and vessels
- Thrombosis / embolism
Specific risks of hip surgery:
- Infections in the area of the implanted hip prosthesis (low lifetime risk).
- Hip dislocation (dislocation of the joint)
- Calcification / calcium inclusions in the surrounding musculature Adhesions and growths around the hip joint
- Differences in leg length
- Loosening of the prosthesis (long-term, usually due to loss of load-bearing capacity of the bone)
After surgery
Stitches are removed about 12 to 14 days after surgery. The hip operation is followed by rehabilitation. The main aim is to optimize the mobility of the artificial joint and to improve the gait, which is often faulty due to many years of rest and stiffening of the joint, through targeted physiotherapy. How long the rehabilitation phase will last and when the patient can move fully again cannot be said in general terms. For example, recovery after ‘classic’ hip surgery can take many months, as the injuries to the musculature heal very slowly. Minimally invasive hip surgery usually takes a few days before the patient can move independently again. The fine motor skills of the musculature are also preserved. As a result, a safe gait pattern can be achieved again quickly. Overall, the acclimatization phase can take about a year. During this period, unaccustomed sensations, noises, or sensitivity to the weather may still occur in the hip area. Depending on the profession and the surgical method, the patient can return to work after 2 to 3 months.
Disclaimer
Please note that this quiz is not a substitute for a professional medical evaluation. If you are experiencing hip pain or discomfort, please consult your doctor or a qualified medical professional.